What is Abuse Amnesia?
Abuse amnesia can take place in many different types of relationships, if the person is abusive, such as with parental figures, romantic partners, with friends or work colleagues. Abuse amnesia can be described as an adaptive behaviour which is caused by growing up in an abusive household. There are psychological and physiological reasons for this phenomenon.
Psychologically, abuse causes children to learn to:
- Zone out – to stop paying attention, to imagine/daydream or think about something else or think about nothing
- Blame themselves
- Fantasise about the ways in which life could be better
- Rationalise things away – trying to find reasons and explanations for what is happening
- Minimise – its not that bad and others have it worse
- Deny completely what is happening
- Believe they deserve to be treated that way
- Defer to other people’s opinions as they cannot trust their own
- Think they are evil or are a monster
These ways of thinking become repetitive – and then automatic – thought patterns that last into adulthood and this leads people from abusive homes into frequently having blind spots around abuse.
The abuse is a trigger and an automatic response like one of the above is activated. This means ‘red flags’ can be harder to register or hold in mind. Triggered responses are born out of confusion or as a protective device.
If a person is able to recognise that there is something off or abusive or wrong happening, usually, within a few hours or days life has often returned to ‘normal’ and the relationship carries seemingly like nothing has happened. This can even happen in cases where someone has been emotionally or physically abused or there has been infidelity.

Signs of Abuse
The Red Flags
Red flags of abusive behaviours are being:
- insulted and belittled
- dismissed
- controlled
- demeaned
- lied to, gaslit
- isolated from others
- blamed for almost everything while the other person tends to not take any responsibility
- threatened
- physically pushed/attacked/hit
Why are Red Flags Ignored?
Fear of Rejection and Abandonment
The fears of rejection and abandonment rule in a traumatised person and are often the strongest driving forces. Placating these fears in themselves means that fawning and submissive behavioural strategies are often the most dominant.
Self-Doubt
Traumatised people often feel they can’t trust their own perceptions and opinions and there is a lot of self-doubt. Validation of their opinions, perceptions and self-worth is something which exists externally rather than internally and therefore gathered from others.
Core Beliefs
People develop core beliefs over the course of their lives and many of these are developed in the early years and can remain unchanged as in a person’s mind they become facts rather than beliefs. These beliefs then become self-fulfilling prophecies, and some core beliefs which develop in abused people are:
- I can’t cope if I am alone
- I’d rather be abused than be alone
- No one else will want me and I will always be alone if I leave this relationship
- I must deserve this because I am too much, crazy, abnormal etc etc
- If they think I am bad then I must be
- I can’t trust or believe what I think
Black and White Thinking
If a person grows up in an abusive home they may not have been able to develop whole and realistic ways of seeing others. They may have black and white thinking patterns such as; “I am all bad” or “I am all good” or another person is “all bad” or “all good.” Flipping between these opposing ways of thinking is confusing and muddies the waters. (Please see whole object relations).
The Trauma Bond
The trauma bond can make it harder to leave. For many people, clinging and dependent behaviours feel ‘good’ as does meeting other people’s needs, and being independent and autonomous feels ‘bad.’ This can be the case even for people who are very self-reliant and do not like to ask for help. This can be a subconscious process which a person does not even realise is happening.
I Deserve It – Lack of Self-Compassion
A person who grows up in a narcissistic family learns to repress self-compassion and positive self-regard as part of their defences. This is necessary in order to be able to put the needs of others first and repress their own. They have learned that having needs or wants or asserting themselves gets met with emotionally or physically violent responses. Others people’s needs and wants have to be valued more than themselves to keep them safe.
The Need to Attach
The need to attach to parental figures, even if they are abusive, is a driver for survival. We repeat the way we attach to our parental figures with others throughout our lives. Much research has been done on attachment styles and trauma and it shows that fearfully attached individuals are more likely to interpret events as stressful and show higher levels of depression, distress, and post traumatic stress symptoms.
A disorganised attachment style (the most common style a person from a narcissistic family will have but not always) is associated with later psychological difficulties and dissociative experiences.
Fantasising
Hope that things will get better can be a strong driver in behaviour. Hope and fantasy are vital coping mechanisms which help a child survive the bleakness.
To fantasise is to live for the future and believe that:
- in a romantic relationship – their partner and the relationship has potential
- it will be better one day
- the day will come somehow when they will finally understand me
- If I try harder/look better/give them what they need etc etc my partner/parent will then think I am good enough
- One day they will see how much they are hurting me and then they will stop
These are old patterns of thinking that have been there since childhood when a child tried to cope with their situation.
What Happens in the brain to cause Abuse Amnesia?
There is also a physiological component to the way people respond to abuse.
Abuse amnesia is also caused by the chain of chemicals that are released in the brain in certain situations:
“When an abusive incident happens, the hormones cortisol and adrenaline are released, putting the individual in a heightened sense of readiness. After extensive incidents of abuse, the brain response has familiarized with a pattern: hyperarousal (abuse and abandonment) and then relief. During the hyperarousal phase, the individual experiences increased levels of stress hormones. Once things have calmed down, the body searches for relief.
During the abandonment phase of the cycle, the victim’s brain releases chemicals that cause the feelings of longing, anticipation, and the motivation to find relief. Endogenous opioid withdrawal causes pain, and the neurotransmitter dopamine motivates the person to search for relief in the object of desire—the abuser.
Once the chaotic encounter between victim and abuser is over, homeostasis sets in. The abusive relationship has become a system. All systems strive for homeostasis, which occurs at a state of equilibrium. Each person in the system adjusts in order to reach that “perfect” state of equilibrium. Abuse amnesia is an essential component of this balance.
It is distressing to think bad thoughts about a recent traumatic event.”
This information is taken from an article at Good Therapy. Please see here: https://www.goodtherapy.org/blog/abuse-amnesia-why-we-stay-with-our-abusive-partners-1003175
Other Types of Amnesia
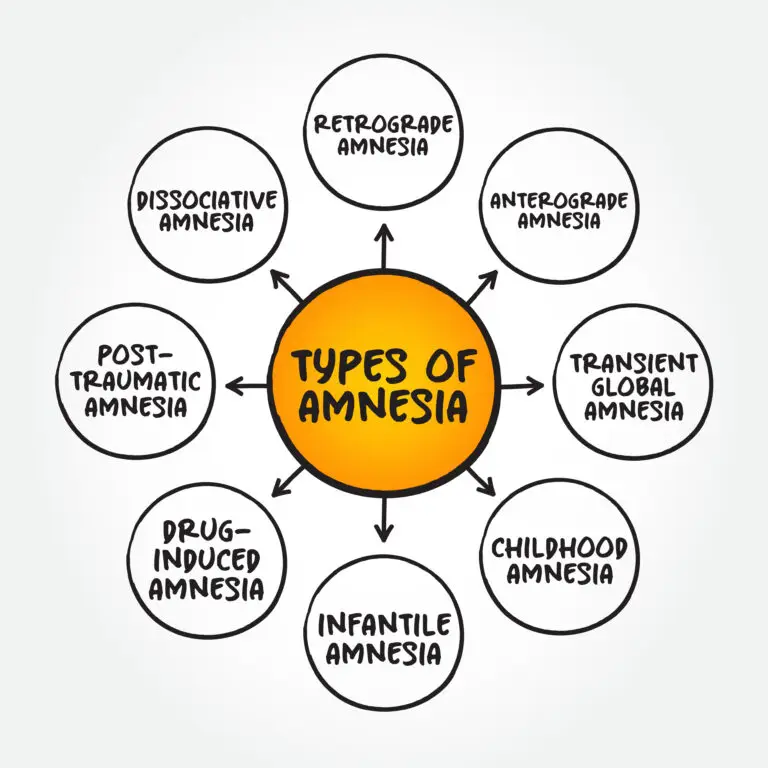
Childhood/Infantile Amnesia
Childhood or infantile amnesia is the inability to be able to remember much before the age of around 3 years old. Some theories say that this is due to immature structures brain that are related to memory, or that the memories are not stored in the long term memory, or that the memories were not verbally encoded so there are no verbal cues that can trigger the memory. Most children start to remember things from around age 3 and a half. Adult-like episodic memory starts to emerge around the age of 6 and develops until adolescence in relation with adult-like hippocampal maturity. Episodic memory is a type of long-term memory that involves the recollection of personal experiences or events, including the time and place that they occurred.
Dissociative Amnesia
Dissociative amnesia can be defined as an inability to recall significant autobiographical information, usually of a traumatic or stressful nature and this helps the person to distance themselves from the pain and distress. This memory loss is not caused by a medical condition or substance use. It can take different forms such as:
- Localised – being related to a specific event
- Selective – which is partial memory loss
- Generalised – which is a complete loss of identity and life history
- Systematised – which means the amnesia is related to a specific category
- Continuous – the inability to form new memories after a traumatic event
Dissociation and Trauma
Dissociation and Trauma can be seen here:
Dissociative Disorders symptoms and DSM-5 and ICD-10 diagnoses
Drug-induced Amnesia
Drug-induced amnesia is a type of memory loss caused by the use of certain drugs, often resulting in an inability to form new memories. This condition can be temporary and is commonly associated with excessive alcohol use, sleeping pills like Ambien, MDMA and GHB, anaesthetics like Ketamine and benzodiazepines like Xanax and Valium.
There are 2 types of blackout associated with alcohol use, the first is a partial blackout, also known as a greyout or a brownout, when memory is spotty with parts missing and the other is known as an ‘en bloc’ where there is a complete blackout where memories do not form and can therefore never come back. These happen when people have a rapid rise in blood alcohol concentration from drinking on an empty stomach or binge drinking. Blackouts can happen at a lower blood alcohol level when certain sleep or anti-anxiety medications are consumed at the same time.
The effects of drug-induced amnesia are mostly temporary and when the substance wears off the brain continues to function normally. However, with prolonged, chronic use the brain can become damaged and this can be permanent.
Post-Traumatic Amnesia
Post-traumatic amnesia occurs following an injury or accident when there has been damage to the brain. One of the symptoms is the loss of memory for the present time. There may be recognition of family and friends but an inability to process the fact that they are in hospital or have had an injury. The condition may last for minutes, hours, days or even or months.
Retrograde Amnesia
Retrograde amnesia can occur following a psychiatric illness or a brain injury. This type of amnesia can be temporary or permanent and affects a person’s ability to access past experiences and knowledge.
Anterograde Amnesia
This type of amnesia is the inability to form new memories. It can result from a brain injury, neurodegenerative conditions and some medications. It affects a person’s ability to learn new information and skills. In most cases of anterograde amnesia, patients lose explicit memory, or the recollection of facts, while retaining procedural memory.
Sources
Abuse Amnesia
https://www.goodtherapy.org/blog/abuse-amnesia-why-we-stay-with-our-abusive-partners-1003175
Self-Fulfilling Prophecy In Psychology: Definition & Examples
https://www.simplypsychology.org/self-fulfilling-prophecy.html
Childhood or Infantile Amnesia
https://www.sciencedirect.com/topics/neuroscience/childhood-amnesia
Episodic Memory
Dissociative Amnesia
https://www.psychologytoday.com/us/conditions/dissociative-amnesia
https://www.apollohospitals.com/diseases-and-conditions/dissociative-amnesia
Drug-induced Amnesia
Post-Traumatic Amnesia
Retrograde Amnesia
https://www.sciencedirect.com/topics/psychology/retrograde-amnesia
Anterograde Amnesia
https://en.wikipedia.org/wiki/Anterograde_amnesia
National Institute on Alcohol Abuse and Alcoholism